 Dr. Rhett Drugge is a native of Darien, Connecticut and a graduate of Harvard University. Graduating with a baccalaureate degree in Intellectual History, he went to Washington DC and wrote senatorial speeches for Connecticut Senator Lowell Weicker. A few years later, he distinguished himself in medical research at Yale University by discovering the receptor for cyclosporin A (the major drug for organ transplant patients). He then matriculated to New York Medical College in Valhalla, New York where he went on to receive his medical degree. While a medical student, he served some of his medical rounds at Stamford Hospital. He completed his medical internship at New York University and then served his Dermatology Residency at the University of Michigan.
Dr. Rhett Drugge is a native of Darien, Connecticut and a graduate of Harvard University. Graduating with a baccalaureate degree in Intellectual History, he went to Washington DC and wrote senatorial speeches for Connecticut Senator Lowell Weicker. A few years later, he distinguished himself in medical research at Yale University by discovering the receptor for cyclosporin A (the major drug for organ transplant patients). He then matriculated to New York Medical College in Valhalla, New York where he went on to receive his medical degree. While a medical student, he served some of his medical rounds at Stamford Hospital. He completed his medical internship at New York University and then served his Dermatology Residency at the University of Michigan.
Board Certified in both Dermatology and Dermatologic Surgery in 1992, Dr. Drugge is a member of the Society for Investigative Dermatology, the American Academy of Dermatology, and the American Society for Mohs Surgery. He is the founder of the Internet Dermatology Society and he is the Chief Editor of the Electronic Textbook of Dermatology. Dr. Drugge has written numerous database information systems for networked medical record keeping, with a special focus on physician to physician communications & dermatology information systems. He also designs and tests imaging solutions for the skin care industry.
In 2008 Dr. Drugge was granted a patent for his unique invention, the Melanoscan system for whole body imaging, which aids in the early detection of skin cancers. He is also active in interviewing prospective undergraduates for Harvard.
Dr. Drugge and his wife Heather live in Darien with their three children.
Specialty Certification
Professional Affiliations

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
1992 Originated “store and forward” text plus image consultations in which have become the standard of care in teledermatology for the largest hospital system in the world, the Veteran’s Administration, and the major backbone of peer-to-peer education in dermatology.
1993 Participated in the interface design of the Dermatology Online Image Atlas with Andy Bittorf, Thomas Diepgen, Thomas Ray and Arthur Huntley.
1994 Recommended that clinical dermatology email lists should be used primarily as a method of case discussions.
1994 Created Global Dermatology Grand Rounds, the first web based interactive dermatology case discussions.
1995 Founded the first online medical society, the Internet Dermatology Society.
Published the first medical textbook on the Internet, the Electronic Textbook of Dermatology.
1996 Presided over the first meeting of the Internet Dermatology Society, now in its 5th year.
1997 Produced the first online dermatology meeting with streaming video.
1999 Published a definitive study showing the equivalence of store and forward teledermatology to traditional dermatology in the JAAD.
2000 Created a systematic Dermatology Quality Index for the 5th Annual meeting of the Internet Dermatology Society.
Curriculum Vitae
Rhett J. Drugge, M.D.
50 Glenbrook Road
Stamford, CT 06902
tel: (203) 324-5719
fax: (203) 323-7485
Rhett.Drugge@snet.net
Scientist, inventor, editor, and consultant in the private practice of dermatology and cosmetic surgery
Harvard College, Cambridge, Massachusetts, A.B. 1977-81
New York Medical College, Valhalla, New York, M.D. 1984-88
Medical Internship: New York University – 1988-89
Chief of Service: Norton Spritz, M.D.
Dermatology Residency: University of Michigan, 1989-1992
Chief of Service: John J. Voorhees, M.D
CME 1997-1999
Practical Skin Pathology Conference in New York City (32 credits)
Winter Skin Seminar (1996) Vail, CO (20 credits)
AAD Annual Meeting (1996) Washington, D.C. (32 credits)
AAD Summer Meeting (1996) Orlando, FL (32 credits)
SID Annual Meeting (1996) Washington, D.C. (15 credits)
American Society for Phlebology Meeting (1996) Washington, D.C. (10 credits)
American Society for Mohs Micrographic Surgery (1996) San Diego, CA (20 credits)
Melanoma 1997, Scripps Clinic, La Jolla, CA (18 credits)
Winter Skin Seminar (1997) Aspen, CO (21 credits)
SID Annual Meeting (1997) Washington, D.C. (15 credits)
AAD Annual Meeting (1997) San Francisco, CA (15 credits)
Army Pathology Institute Course (May 1997) Washington, DC (15 credits)
AAD Summer Meeting (July 1997) New York, NY (10 credits)
ADC Conference (October 1997) New York, NY (15 credits)
American Society for Mohs Micrographic Surgery (1997) San Diego, CA (20 credits)
AAD Annual Meeting (March 1998) Orlando, FL (15 credits)
AMIA Conference (1998) Nashville, TN (10 credits)
Army Pathology Institute Course (May 1998) Washington, DC (15 credits)
ASDS Annual Meeting (May1998) Portland, OR (21 credits)
ASCS Cometic Surgery Course: Liposuction Congress (October 1998), Anaheim, CA (10 credits)
ADC Conference (October 1998) New York, NY (13 credits)
BU Course: Hands on Reconstruction November 1998) Boston, MA (18 credits)
Harvard Course: Melanoma (November 1998) Boston, MA (20 credits)
AAD Annual Meeting March 1999 New Orleans, LA (40 credits)
IDS Annual Meeting March 1999 New Orleans, LA (5 credits)
7/92 – Present
Remote Access Dermatology Research.
Member of the American Academy of Dermatology Telemedicine Interest Group and the President’s Special Committee on Technology.
Founder, The Internet Dermatology Society.
Founder and Chief Editor, Global Dermatology Grand Rounds, an Internet based forum for exchange of challenging dermatology cases.
Telemedicine Editor, Dermatology Online Journal.
Milestones
May, 1993 – initiated remote access service to St. Joseph Family Medicine Center for the purpose of enhancing family practice residency training.
December, 1994 – founded Global Dermatology Grand Rounds, an Internet-based high-level teledermatology application.
February, 1995 – founded the Internet Dermatology Society.
August, 1995 – produced the web site for the Society for Investigative Dermatology.
September, 1995 – demonstrated the use of the web as an organizing structure for off-line dermatology lectures to primary care physicians using materials from the Electronic Textbook of Dermatology.
July, 2000 – submitted a patent on Total Immersion Photography for Skin Disease Documentation.
11/89 – 3/90
Research associate, University of Michigan, Immunoprecipitation of phosphotyrosinated substrates of epidermal growth factor receptor. Sponsor: J.T. Elder, M.D. Ph.D.
10/85 – 9/86
Research associate, New York Medical College, part-time from October to May studying immunofluorescent staining and cytolytic assays with lymphokine-activated natural killer (LANK) cells; full-time, from June to September, performing c-DNA library screening for the nucleotide sequence of perforin-1, a component of LANK cell granules. Sponsor: E.R. Podack, M.D.
7/85 – 8/85
Summer student fellowship, New York Medical College, studying the influence of the cyclosporin A binding protein, cyclophilin, on mitogen stimulated human peripheral blood lymphocytes. Co-sponsors: J.W. Chiao, Ph.D. and R.E. Handschumacher, Ph.D.
11/82 – 8/84
Research assistant, Yale University School of Medicine, isolation and purification of cyclophilin, the putative receptor for cyclosporin A. Cyclosporin A metabolite studies. Sponsor: R.E. Handschumacher, Ph.D.
Presentations and Publications
Latest Publication: J Am Acad Dermatol 1999 Nov;41(5 Pt 1):693-702
Reliability and accuracy of dermatologists’ clinic-based and digital image consultations.
Whited JD, Hall RP, Simel DL, Foy ME, Stechuchak KM, Drugge RJ, Grichnik JM, Myers SA, Horner RD
Institute for Clinical and Epidemiologic Research, Veterans Affairs (VA) Medical Center, Durham, North Carolina 27705, USA.
BACKGROUND: Telemedicine technology holds great promise for dermatologic health care delivery. However, the clinical outcomes of digital image consultations (teledermatology) must be compared with traditional clinic-based consultations. OBJECTIVE: Our purpose was to assess and compare the reliability and accuracy of dermatologists’ diagnoses and management recommendations for clinic-based and digital image consultations. METHODS: One hundred sixty-eight lesions found among 129 patients were independently examined by 2 clinic-based dermatologists and 3 different digital image dermatologist consultants. The reliability and accuracy of the examiners’ diagnoses and the reliability of their management recommendations were compared. RESULTS: Proportion agreement among clinic-based examiners for their single most likely diagnosis was 0. 54 (95% confidence interval [CI], 0.46-0.61) and was 0.92 (95% CI, 0. 88-0.96) when ratings included differential diagnoses. Digital image consultants provided diagnoses that were comparably reliable to the clinic-based examiners. Agreement on management recommendations was variable. Digital image and clinic-based consultants displayed similar diagnostic accuracy. CONCLUSION: Digital image consultations result in reliable and accurate diagnostic outcomes when compared with traditional clinic-based consultations.
J D Whited, B J Mills, R P Hall, R J Drugge, J M Grichnik and D L Simel
A pilot trial of digital imaging in skin cancer, Journal of Telemedicine and Telecare, April 1998.
A. Bittorf, N.C. Krejci-Papa, T. Ray, A. Huntley, D.C. Collison, R. Drugge, D. Hiller, M. Bergmann, T.L. Diepgen1, Applications of the WWW: A Multicentered Dermatologic Image Database, poster presentation, 3rd WWW Conference, May 1995.
Chan, LS, Fine, JD, Briggaman, RA, Woodley, DT, Hammerberg, C, Drugge, RJ, Cooper KD, Identification and partial characterization of a novel 105-kDalton lower lamina lucida autoantigen associated with a novel immune- mediated subepidermal blistering disease.: J Invest Dermatol (1993 Sep) 101(3):262-7
Elder, JT, Pepinsky, RB, Drugge, RJ, Voorhees, JJ, Wallner, B, Increased expression of lipocortin I mRNA, but not lipocortin I protein, in psoriasis. poster presentation, Society of Investigative Dermatology, May 1990.
Drugge, RJ, Handschumacher, RE, Cyclosporine: mechanism of action. Transplantation Proc., Vol. XX, No. 2, Suppl 2: 301, 1988.
Handschumacher, RE, Harding, MW, Rice, J, Drugge, RJ, Speicher, DW, Cyclophilin: a specific cytosolic binding protein for cyclosporin A. Science, 226: 544, 1984.
Internet Web-based publications (currently active)
Electronic Textbook of Dermatology, R.J. Drugge, Founding Editor and Publisher, 1995-present.
Dermatology Online Journal, Internet Editor, R.J. Drugge, 1996-present
We now offer gift certificates for facial treatments.
You may purchase one certificate for $100 or three for $250.
To purchase a gift certificate please call us at (203) 324-5719
Are Botox treatments safe?
Botox injections have been used safely and effectively for over ten years to treat many ophthalmological and neurological disorders. Each year thousands of patients receive Botox treatments for a variety of conditions and it has become a popular treatment for reversing the visible signs of aging. Dynamic wrinkles are caused by contractions of the delicate underlying facial muscles every time you smile, laugh or frown. The more emotion you show, the deeper these wrinkles and lines are likely to be. While you may have earned every one of your worry lines, you don’t have to show them anymore.
What is “Botox”?
Botulinum toxin (Botox) is a protein produced by a bacteria called Clostridium botulinum. The effects that this toxin can have on the body have been known since the turn of the century, but in the 1980’s the beneficial, cosmetic effects of Botox were discovered, and turned to our advantage. Botox has a relaxing effect on muscle tissue, thus when it is injected into specific target areas of certain muscle groups those muscles lose some or all of their ability to contract.
How can Botox help me?
Take a look in the mirror and frown at yourself. See where the vertical furrows develop between your brows? Now relax. Can you still see remains of those furrows? Now squint at yourself. See the crows feet develop around your outer eyes? Again, relax. Can you still see where those lines were? If you answered yes to either of those questions then Botox may be helpful to you. The permanent presence of frown lines or crows feet may be due to the over-activity of certain muscle groups. Over time this causes deep wrinkles or furrows to appear, which may result in a prematurely old appearance, or a less than pleasant expression. The injection of Botox into those muscle groups on the forehead and/or around the eyes can help eliminate those furrows, giving a more youthful appearance or a more pleasing demeanor.
What will the results be?
A botox injection can take from 1 to 2 weeks to become fully effective but most people notice the effect within 48 hours. During this period a subtle relaxation of the muscle takes place such that you should not even be aware that it has happened – until you notice that the lines are gone! The ability to frown or squint are also reduced. The treatment is not permanent – one of the benefits of botox injections. The effects will slowly wear off – over a time period which can vary from person to person (from 4 to 6 months). Therefore, if you are dissatisfied with the results you can be reassured that it will wear off. Permanent relaxation of the muscle can be achieved after repeated treatments.
Preparation, the Procedure and After-care
There is no preparation that you need to do other than have a consultation with your physician about your suitability for the treatment. The injections themselves are done with the patient in the sitting position, and a very small, fine needle is used to inject a controlled dose of the toxin into specific areas of the target muscles. The procedure takes no more than a few minutes. There is no aftercare required – you may return to work or the rest of your day’s schedule immediately.
What is the price?
The cost per BOTOX® session is $435 USD. Areas that require more than a single injection, such as the area beside the eyes where so-called “crow’s feet” tend to form, can range from $300 to $1000 USD. Larger surface areas such as the forehead can cost as little as $500 and as much as $1400 USD.
Are Restylane treatments safe?
Significant risks with Restylane injections are infrequent, but the potential side effects to the treatment are:
However these side effects listed above usually disappear within two to three days.
Restylane has been proven to be a safe procedure. Since it is non-animal based, it virtually eliminates the possibility of disease transmission or an allergic reaction. Plus Restylane is biocompatible with human hyaluronic acid.
What is “Restylane”?
Impressions of beauty change with time – as do our faces as we age. With RESTYLANE, you can have a natural beauty lift with the body’s own material. RESTYLANE is a crystal-clear, non-animal, biodegradable gel based on a natural substance, called hyaluronic acid. The gel is injected into the skin in tiny amounts with a very fine needle. The result is instantaneous and produces a long-lasting,natural enhancement, gentle and safe to your skin.
Where Can Restylane Be Used?
Hyaluronic acid implantation can be used to improve the skin’s contour and reduce depressions in the skin due to scars, injury or lines.
Facial lines and features that can be corrected using these hyaluronic acid fillers are:
How long will the procedure take?
The Restylane injections can take anywhere from a few minutes to an hour, depending on how large of an area needs to be treated.
Another Restylane benefit is that the procedure is completed quickly, so the patient can have it done during a lunch hour. Go to lunch, have the Restylane procedure, and return to work looking younger.
Preparation, the Procedure and After-care
Achieving the look you desire is as easy as it is quick. The result is instantaneous. No previous skin test is needed, which means that you can have the treatment immediately. The session often takes less than thirty minutes. The time differs somewhat depending on the desired correction. During treatment, RESTYLANE is injected into the skin in tiny amounts with a very fine needle. When injected, RESTYLANE produces volume that smoothes the wrinkle or fold, shapes the facial contour or enhances the lips in a natural way. The result is immediate. The method of injecting RESTYLANE is fast, safe and leaves no scars or other traces on the face.
What is the price?
A full Restylane syringe (for e.g., enough to do the lines around the lips) is $500.
Why have a chemical peel?
If your skin is blemished from sun damage, or acne scarring then a chemical peel may be a good remedy for removing the blemishes. Clinical signs of photoaging of the skin include rhytids (wrinkles around the eyes), lentigines (pigmented spots), keratoses, telangiectasia (broken blood vessels), loss of translucency, loss of elasticity, and a sallow color. A consultation with your dermatologist will help determine what kind of peel is best for you, and whether it could be a single treatment or a series of treatments performed over several months.
Chemical peels can effectively improve a wide variety of skin conditions including:
What is a “chemical peel”?
Chemical skin peeling is an established technique for improving or erasing wrinkles, keratoses and areas of increased pigmentation, including freckles, “age or liver spots”, etc. This technique was developed in 1903 by Dr. George Miller McKee – the founder of the practice of Sheard & Drugge.
A chemical peel is the application of an acid to the skin, usually on the face, although any area may be treated. This removes the superficial, damaged layers to reveal new, undamaged skin. The depth of the peel depends on the formulation and the concentration of the acid used. As the procedure has developed, the formulations have greatly improved to allow for a much wider range of desired results – and more comfort and satisfaction for the patient.
What will the immediate results be?
This would depend on the type and strength of the peel done. A mild peel may produce little immediately discernible effects – the effect is more noticeable once the skin layers treated by the acid have sloughed off, usually in a few days. A deeper, more concentrated peel may produce redness that lasts for a couple of weeks, this will gradually fade to reveal the fresh, undamaged skin. A strong, one-step peel can result in what appears to be a second degree burn – intense redness, some blistering. This can last for up to a month or so, until the new layers come up – these strong peels have the worst short-term effects, but produce the best long-term results for badly blemished skin.
Preparation, the Procedure and After-care
Your dermatologist may instruct you to prepare your skin in the week or two prior to the peel by using certain skin products. These preparations help to remove dead skin cells which improves the efficiency of the peel. The peel itself is performed as a normal office visit in which the doctor will clean the skin with alcohol, apply the peel and then, depending on the peel used, either water or a special neutralizing agent. You may experience some mild burning and stinging as the peel works into the skin layers, but this is usually very short lived (a few minutes). After care will depend on the strength of the peel, but is usually very simple and straightforward – however, we don’t recommend the use of makeup for a little while, especially for stronger peels. Therefore you need to be prepared to go around looking a little “rough” for a while if you have a stronger peel performed. Your dermatologist can help you decide if a series of milder peels, or one strong peel is better for your individual needs.
What is the price?
The cost of the chemical peel is $90 USD.
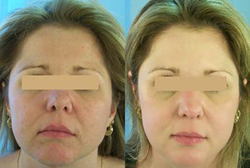 Acne is driven by sebaceous gland secretions, most common in teenagers, but it can also occur in adults and in the first few weeks of life (transplacental hormone influences) and occasionally starts at age 8 or 9. The face, chest and upper back are the most commonly affected sites although acne may be present on the shoulders, arms, underarms, groin and scalp. Acne may induce lifelong scarring and thereby affect a person’s self-esteem. Acne is as a general rule quite curable, excluding those regions in which scarring has been so severe as to cause cyst formations. Even advanced cases can usually benefit tremendously from dermatologic management, from the simple topical home remedies to the most elaborate scar revisions which may include scar subcision, soft-tissue augmentation and skin resurfacing (the latter involving peels, lasers and abrasive techniques). In some cases, entire face lifting as well as botox may be necessary to control the damage to the patient’s sense of esthetic self-esteem.
Acne is driven by sebaceous gland secretions, most common in teenagers, but it can also occur in adults and in the first few weeks of life (transplacental hormone influences) and occasionally starts at age 8 or 9. The face, chest and upper back are the most commonly affected sites although acne may be present on the shoulders, arms, underarms, groin and scalp. Acne may induce lifelong scarring and thereby affect a person’s self-esteem. Acne is as a general rule quite curable, excluding those regions in which scarring has been so severe as to cause cyst formations. Even advanced cases can usually benefit tremendously from dermatologic management, from the simple topical home remedies to the most elaborate scar revisions which may include scar subcision, soft-tissue augmentation and skin resurfacing (the latter involving peels, lasers and abrasive techniques). In some cases, entire face lifting as well as botox may be necessary to control the damage to the patient’s sense of esthetic self-esteem.
Acne is generally earlier in onset and most severe in young men, where as women suffer from a long, slow acne development process. Biologically speaking, acne is driven by androgenic sex hormones, testosterone and androstenedione. Androgen sensitive hair follicles contain the sebaceous glands which thicken the skin of the face, scalp, ears, neck, upper back, chest shoulders and arms. Ensuing sebaceous secretions overwhelm clogged hair follicle outlets (pores). Acne is not typically caused by infection, but it does set the stage for secondary infections. Sebacous glands reflect nature’s attempts to provide protection from the elements that primitive man encountered. At ages 12-14, boys and girls were expected to make their own way and catch their own food so nature provided them with the hormone of aggression, testosterone. In general, estrogens decrease sebaceous gland activity and androgens increase it. In women, androgens are produced by the ovaries (markedly so in polycystic ovary disease), the placenta and adrenals, and in men by the testes and adrenals. While males experience a peak in testosterone at age 18, female testosterone peaks at 31. Birth control pills by their estrogenic effects have a mild effect on acne. It is occasionally noticed that some of the more androgenic preparations may aggravate acne and even produce mild hirsutism. A certain amount of trial and error for each individual is therefore necessary to pick out the best contraceptive.
Did you know?
Effects of Future Weight Gain
The current belief is that once fat cells have been removed from the body they do not grow back. Future weight gains tend to be distributed more evenly over the body, as weight gain is the result of existing cells swelling. Obviously liposuction removes some of those cells, so weight gain in the treated areas is proportional to the increase in size of remaining cells.
What is Liposuction?
Liposuction was developed in the 1970’s by Georgio Fischer, M.D. of Italy for the removal of fat deposits located in areas that are resistant to diet and exercise, or that are naturally subject to fat deposition. While not a treatment for generalized obesity, this procedure is ideal for the removal of unwanted fat deposits in the face, chin, neck, hips, buttocks, abdomen, knees, calves, chest and breasts.
The Best Candidates for Liposuction
To be a good candidate for liposuction, you must have realistic expectations about what the procedure can do for you. It’s important to understand that liposuction can enhance your appearance and self confidence, but it won’t necessarily change your looks to match your ideal or cause other people to treat you differently. The best candidates for liposuction are normal-weight people with firm, elastic skin who have pockets of excess fat in certain areas. You should be physically healthy, psychologically stable and realistic in your expectations. Your age is not a major consideration; however, older patients may have diminished skin elasticity and may not achieve the same results as a younger patient with tighter skin. Liposuction carries greater risk for individuals with medical problems such as diabetes, significant heart or lung disease, poor blood circulation, or those who have recently had surgery near the area to be contoured.
Preparation, Surgery and Immediately Afterwards
Planning and discussion of liposuction may require one or two consultations before an appointment for the procedure is made. A consent form will be signed by the patient prior to treatment. Prior to having the surgery, patients should refrain from taking any aspirin, (it can interfere with proper blood clotting for at least 10 days).
On the day of the surgery, you may go about your usual routine, eat a light breakfast if the surgery is in the morning or a light lunch if it is in the afternoon. Avoid drinking large quantities of liquid, as the procedure may take 1-3 hours. Be on time for your appointment and wear comfortable loose-fitting clothes. Pre-operative digital photographs will be taken prior to the procedure.
At the surgery, the doctor will mark the areas to be treated and inject local anaesthetic into the areas where he plans to make incisions. Small incisions are then made through which saline and numbing solution will be injected using a blunt-tipped needle. Some discomfort may be felt initially as the solution starts to go in, but that should soon fade as the anaesthetic takes effect. The doctor will inject the solution across the entire area to be treated. (Patients report a feeling more of pressure than discomfort or pain during this). Then, the doctor will insert the instrument (cannula) and start to remove the fat through suction.
You will work with the doctor during the procedure and he will ask you to stand up to assess the smoothness of your new contours (fat lies differently in different positions). If the procedure is on the buttocks, legs or abdomen, we request that you have someone to drive you home and also recommend taking it easy for the first 24 hours, but there is no need to stay completely sedentary. In fact, light activity will help to stimulate healing. Post-operative bruising and discomfort is usually minimal and may be treated with low grade pain-killers such as Tylenol.
A follow up visit two days later is scheduled. You should not expect to be fully able to assess the results for a few months, as the skin recontours to the reduced fat layer. In a month, additional photographs will be taken to compare to the pre-operative photos.
What is the cost of liposuction?
Body site Surgical Fee(US$)
Abdomen, upper & lower $3,000
Arms $2,000
Back $4,000
Breasts, female $2,500
Breasts, male $2,500
Buttocks $2,500
Chin, Cheeks, Jowls, Neck $2,000
Flanks $3,000
Outer Thighs $3,000
Inner Thighs $3,000
Hips/Waist $3,000
Ankles & Knees $2000
Spider veins, or telangiectasias, are those tiny purple and red blood vessels found most commonly on the thigss or lower legs of women. They are hereditary and can form anywhere on the leg, from the top of the thigh to the ankle. Occasionally, spider veins appear on the face.
Varicose veins are larger. They can appear raised, with a bluish color, and can become quite painful. Although spider veins and varicose veins carry blood, they are not part of the venous valve system.
Spider veins are most often treated with sclerotherapy, in which a saline or chemical solution that is injected into the vein, irritating the lining and causing the vein to collapse and disappear.
In some cases, laser treatment may be used either alone or in combination with sclerotherapy.
Did you know?
4. Dr. Drugge was trained in liposuction in his residency and has been performing this safe technique for over ten years.
How is it done?
The softness and suppleness which give the breasts their shape are due mainly to the presence of adipose tissue (fat). Natural Breast Augmentation is an injection technique used to transfer natural adipose tissue from one area of the body to the breasts.
The tissue is alive and as such is treated like a graft. Volumetric measurements of the breasts are taken before each injection series and the adipose tissue is injected in the precise proportion necessary for the greatest survival. The tissue that is retained after three months is considered permanent.
The procedure requires a small extraction (mini-liposuction) procedure from the outer thighs, hips, buttocks, or abdomen. This is done under local anesthesia.
The collected adipose tissue is frozen at -30 C. Some blood is taken for laboratory processing where the platelet enriched plasma is added back to the tissue before injection.
Once the breasts are numb with local anesthesia through a 4mm hole under each breast, the enriched adipose tissue is injected using a blunt cannula into the specific areas of the breasts which need enhancement. The most popular areas for injection are the upper quadrants of the breast which enhance the roundness of the breast and the appearance of cleavage. This technique can also improve breast assymetry.
The breasts are then enlarged gradually over several injection series depending upon the cup size desired. For further information about the procedure, please request a lipsuction pamphlet from Dr. Drugge’s office.
Who is the ideal candidate for NBA?
Small breasts (A cup/B cup) or flat breasts.
Available adipose tissue from another part of the body such as the thighs, hips or abdomen. (Until we develop a way to grow your adipose tissue in vitro, you must have adequate harvest material.)
Pre and Post Procedure Details
Planning and discussion of the harvest and injection procedures may require one or two consultations before an appointment for the procedure is made. Prior to having the surgery, patients should refrain from taking any aspirin, (it can interfere with proper blood clotting for at least 10 days).
Be on time for your appointment and wear comfortable loose-fitting clothes. Pre-operative digital photographs will be taken prior to the procedure.
Bring a sports bra or underwire bra to wear after the procedure. Post-operative discomfort is usually minimal and may be treated with low grade pain-killers such as Tylenol. There may be minimal (1-3 teaspoons) of leakage from the incision holes over the next 24 hours from the anesthesia. This can be pink or yellowish in color.
The patient should not expect to be fully able to assess the results for a few months, as the skin recontours to the enhanced fat layer. In a month, more photographs will be taken to add to the patient’s record and be compared to the pre-operative photos.
Effects of Future Weight Gain or Loss
Since the breasts are sensitive to weight loss, it is not recommended to diet or lose weight. Adipose tissue will shrink with weight loss and swell with weight gain. Some patients have experienced increased breast size on top of the procedure with minimal weight gain.
What is a Melanoscan?
A Melanoscan is created by taking a series of photographs of the skin surface of a patient which can then be examined individually or as a composite. It is a technique used by dermatologists that provides them with a record of existing skin lesions and gives them something to compare the appearance of new lesions against, rather than just having to rely on either their own, or the memory of the patient, as to when a mark first appeared on the skin and its subsequent changes in size, color, etc.
The ability to identify new marks or lesions in a timely fashion has a major impact on the efficiency of the management of skin cancer. Through early detection, removal of any cancerous lesions becomes much less destructive both physically and emotionally. Advances in technology (e.g. the use of digital cameras to produce images on a computer screen) have greatly enhanced our ability to recognize both pre-existing and newly emergent skin lesions by providing better image manipulation (including magnification to aid the human eye) and allowing side-by-side comparisons of pictures taken over a period of time.
Who should have a Melanoscan?
What is the procedure?
If in consultation with your dermatologist you decide that you are a candidate for a Melanoscan, then an appointment will be scheduled at a convenient time for you. The process of taking the serial pictures of the body takes approximately 15 minutes. You will be asked to disrobe (we will provide you with disposable underwear, if you wish). A series of pictures in three choreographed positions will then be captured in our completely private Melanoscan booth – the automated instructions will direct you through each simple step of the procedure. To facilitate the process we ask that ladies do not wear any makeup, any long hair is pulled up, and that watches and jewelry are removed.
After the images are captured, the dermatologist will examine you in the areas that are hard to image such as the oral cavity and the scalp. After the appointment, your dermatologist will review the images, and if anything is considered to need further attention you will be notified. Your dermatologist will recommend an appropriate time frame after which another series of images will be taken.
For more information on the revolutionary Melanoscan technology you may visit melanoscan.com
Introduction:
Mohs Micrographic Surgery is a specialized procedure for the removal of skin cancer. The procedure is named after the originator of the technique, Dr. Frederick Mohs. This information packet was written to help you understand what Mohs Micrographic Surgery is, and why it is recommended for the treatment of skin cancer.
Rhett Drugge, M.D., is board certified as a dermatologist by the American Board of Dermatology and Dermatologic Surgery and is a fellow of the American Society for Mohs Surgery.
Dr. Drugge is one of a very small number of specially trained dermatologists who performs Mohs Micrographic Surgery in this region. This highly successful surgery is offered in an outpatient setting at the dermatology office of Dr. Charles Sheard and Dr. Rhett Drugge on 50 Glenbrook Road in Stamford, Connecticut. Patients who undergo Mohs Micrographic Surgery do so in relative comfort and do not require a hospital visit.
Dr. Drugge encourages patients to be as informed as possible about the surgical procedure they are considering. He and his staff are available to answer any questions you might have.
What is skin cancer?
Skin cancer, by far the most common malignant tumor in humans, is an abnormal growth of cells that expands in an unpredictable pattern on the skin. The most common types of skin cancer are basal cell carcinoma, squamous cell carcinoma, and malignant melanoma- each named for the particular skin cell from which it arises. Basal cell carcinomas and squamous cell carcinomas are commonly treatedby Mohs Micrographic Surgery in our office. Other types of skin cancer can also be treated with Mohs Micrographic Surgery.
Both basal cell carcinoma and squamous cell carcinoma begin as a single point in the upper layers of the skin and slowly enlarge, spreading both along the surface and downward. These extensions cannot always be directly seen. The tumor often extends far beneath the surface of the skin. If not completely removed, both types of skin cancer may invade and destroy structures in their path.
Although these skin cancers are locally destructive, they do not metastasize (spread) to distant parts of the body. Metastasis is extremely rare in basal cell carcinoma and usually occurs only with long-standing, large tumors. Squamous cell carcinoma is slightly more dangerous and patients must be observed for any spread of the tumor, although it is unlikely. Certain types of melanoma are treated by Mohs Micrographic Surgery in our facility.
What causes skin cancer?
Excessive exposure to sunlight is the single most important factor associated with the development of skin cancers. In addition, the tendency to develop these cancers appears hereditary in certain ethnic groups, especially those with fair complexions and poor tanning abilities. Fair-skinned people develop skin cancers more frequently than dark-skinned people and the more sun exposure they receive, the more likely they are to develop a skin cancer. Other factors, including exposure to certain chemicals, may also be involved in the development of skin cancers. But the highest incidence of skin cancer is found in cities such as Dallas and Miami where the sun is very intense.
How is skin cancer treated?
There are several methods for treating skin cancers, including excision (surgical removal), curettage and electrodesiccation (scraping and burning), X-ray therapy, cryosurgery (freezing), topical chemotherapy and Mohs Micrographic Surgery. The method chosen depends on the location of the cancer, its size, type, and previous treatment. Your doctor will base his recommendations on these factors.
What is Mohs Micrographic Surgery?
Approximately 40 years ago, Dr. Frederick Mohs of Madison, Wisconsin developed a unique treatment of skin cancer called chemosurgery. Dr. Mohs applied a caustic chemical to “fix” (harden) the area involving the area involving the tumor, so that it could be removed and traced to all of its edges. Since then, the procedure has been refined. Today, almost all cases are treated by the “fresh tissue” technique which omits the use of this caustic chemical and allows dermatologists to remove all of the tumor layers in one day. Mohs Micrographic Surgery is a technique that enables dermatologists to selectively remove areas involved with the skin cancer, while at the same time preserving the greatest amount of normal tissue as is possible. If surgical repair of the defect is necessary, it can be done with the knowledge that there is no residual tumor left. As a result, Mohs Micrographic Surgery is very, very useful for large tumors, tumors with indistinct borders, tumors near vital functional or cosmetic structures and tumors for which other forms of therapy have failed.
What will happen at my preoperative visit?
Your first visit allows the doctor an opportunity to examine your skin cancer, obtain your medical history and determine whether the technique of Mohs Micrographic Surgery is the most appropriate treatment. It also gives you a chance to meet Dr. Drugge and his staff and learn about the procedure. If you have been referred to the office, we will usually have received a pathology report stating the type of skin cancer you have. If this information has not been obtained, we will perform a biopsy during your preoperative visit. This biopsy is important because it will tell us what type of cancer you have – a critical factor in planning your treatment. The date and time of your surgery will also be scheduled at this consultation.
How should I prepare for surgery?
Eat your usual breakfast. If you normally skip breakfast, please have a morning snack on the day of surgery.
Take all of your regular medications unless directed otherwise by your surgeon or your regular physician. If you take any medicine containing aspirin, salicylates, other pain medicine, anti-inflammatory medicine or arthritis medicine, please discuss this with Dr. Drugge.
Wear comfortable, loose-fitting clothing that you can easily get into and out of. Avoid any pull-over clothing. If necessary, we may give you a hospital gown to wear during your surgery. You may also want to bring a sweater in case the clinic room is air-conditioned.
Please leave your whole day available for surgery. That will allow enough time for you to rest and recover from the procedure. On the day of your surgery, we encourage you to bringa close friend or relative with you who can help you drive home and keep you company between each stage of the procedure.
If you are very anxious or nervous, we can give you a mild sedative prior to surgery. This must be arranged prior to the day of surgery. If you take a sedative, you must be accompanied by a close friend or relative who can take you home after your surgery.
How is surgery performed?
Mohs Micrographic Surgery is performed in a procedure room under sterile conditions, with local anesthesia. Once anesthesia is complete, the visible portion of the tumor is removed by excision or scraping with a sharp instrument called a curette. Following the removal of most of the tumor, a thin layer, encompassing the complete undersurface of the tumor, is excised. That layer is then cut into small pieces and a map is drawn to identify the location of each piece. The edges of each piece are marked with dyes to aid in orientation on our map. Each piece is then frozen and these slices cut, stained, and examined under the microscope. Any areas in which the tumor is found are marked on the map. Regions with remaining tumor tissue are then reexcised. This procedure is repeated until no more tumor is found and the cancer is entirely removed. After each layer of tissue is obtained, oozing or bleeding vessels are cauterized or ligated with a suture. A pressure dressing is applied. You may then rest in a specially equipped waiting area with your family member or friend.
How long does it take?
It takes 30 minutes to remove each layer of tissue, and one or two hours to process and examine it. Most tumors require the removal of three layers. Extensive tumors may need more surgery and may require a second visit.
Will Mohs Micrographic Surgery cure me?
If you have a basal cell carcinoma, there is about a 99 percent chance that you will be cured. If you have a squamous cell skin cancer, you can be about 95 percent certain that you will be cured by Mohs Micrographic Surgery. However, follow-up visits to detect the rare recurrence are very important. After the initial postoperative period, you will return to your referring physician for routine skin care and tumor surveillance. The Mohs surgeon will see you about once each year for five years to rule out the possibility of recurrence.
When will my post-surgical plan be developed?
Since it is not possible to know the exact size of each skin cancer until it has been completely removed, we cannot determine your post-surgical treatment entirely in advance, although we can tell you what to expect. Many wounds are superficial and can heal on their own with excellent cosmetic results. If a surgical wound requires surgical reconstruction, we will discuss it with you following the complete removal of the cancer. Appropriate recommendations and referrals will be made at that time.
What can I expect after the surgery?
You surgical wound will likely require special care during the week(s) following surgery. You will have some swelling and redness around the wound. This will gradually disappear over seven to ten days. In larger wounds, some drainage may occur andmay have a foul odor for a few days. You should plan on wearing a dressing and avoid strenuous physical activity for one to two weeks.
You may experience a sensation of tightness across the area of surgery. Skin cancers frequently involve nerves, and months may pass before your skin sensation returns to normal. In some cases, numbness may be permanent. You may also experience itching after your wound has healed. Complete healing of the surgical scar takes place over 12 to 18 months. Especially during the first few months, the site may feel swollen or lumpy and there may be some redness. Gently massage the area (starting about one month after surgery) and keep the area lubricated with lotion to speed the healing process.
Bleeding
Bleeding is rare. If it occurs, have someone apply firm pressure to the site. If a bulky dressing has been placed on the wound, this should not be removed. Direct pressure should be applied to the padded wound for 15 minutes, timed by watching a clock. Do not discontinue pressure to see if the bleeding has stopped until 15 minutes have elapsed. If the bleeding continues, continue to press directly with an additional clean gauze pad over the bleeding site for another 15 minutes. If bleeding continues, call our office or go to your local emergency room.
Pain
Mild to moderate pain is normal for a day or two following surgery, but it generally responds well to oral pain medications such as Tylenol or Tylenol #3. Do not use aspirin or anti-arthritis pain medications such as Motrin or Advil (ibuprofen) because they can cause bleeding. If regular pain medications provide insufficient relief, or if the pain increases after 3 to 4 days, you should contact our office.
How will my wound heal?
The human body healed itself naturally for thousands of years before the advent of modern medicine, and it has great recuperative ability. After the complete removal of the tumor, several options may be considered for managing the wound.
Healing by spontaneous granulation
Letting the wound heal by itself offers a good chance to observe the healing process and decreases the chance of a recurrent cancer being invisible or hidden. If at any time during the course of healing, the scar is deemed to be unacceptable, a cosmetic surgical procedure can be performed. Allowing wounds to heal this way is relatively painless and offers excellent cosmetic results for many body locations.
Closing the wound or part of the wound with stitches
This procedure often speeds healing and can offer good cosmetic results, especially when the scar can be hidden in a line of facial expression or wrinkling. Sutures generally remain in place for 5 to 7 days, and occasionally up to two weeks, depending on the location. Do not bathe the area for the first 72 hours. On the fourth day following surgery, you may shower, but you must avoid bathtubs and swimming pools for 5 to 7 days.
Closing the wound with skin grafts, flap repairs or other reconstructive procedures
Recommendations or referrals for these procedures will be made after complete removal of the tumor. We will make recommendations that best serve each patient’s needs.
How should I care for my wound?
You can act as your own nurse and will be impressed at the excellent job you can do. To facilitate the healing of your wound, you must change the dressing daily. With proper care you will be surprised and please at how well and rapidly your wound heals. The following materials may be required, but should not be purchased before you receive your postoperative instructions.
How do I change the dressing?
Keeping the dressing fresh and clean will facilitate healing. Follow these steps:
Important reminders:
What about…?
We want you to be as comfortable, relaxed and informed about your Mohs Micrographic surgery as possible. Please call us at (203)324-5719 us if you have any questions.
What is a Melanoscan?
A Melanoscan is created by taking a series of photographs of the skin surface of a patient which can then be examined individually or as a composite. It is a technique used by dermatologists that provides them with a record of existing skin lesions and gives them something to compare the appearance of new lesions against, rather than just having to rely on either their own, or the memory of the patient, as to when a mark first appeared on the skin and its subsequent changes in size, color, etc.
The ability to identify new marks or lesions in a timely fashion has a major impact on the efficiency of the management of skin cancer. Through early detection, removal of any cancerous lesions becomes much less destructive both physically and emotionally. Advances in technology (e.g. the use of digital cameras to produce images on a computer screen) have greatly enhanced our ability to recognize both pre-existing and newly emergent skin lesions by providing better image manipulation (including magnification to aid the human eye) and allowing side-by-side comparisons of pictures taken over a period of time.
Who should have a Melanoscan?
What is the procedure?
If in consultation with your dermatologist you decide that you are a candidate for a Melanoscan, then an appointment will be scheduled at a convenient time for you. The process of taking the serial pictures of the body takes approximately 15 minutes. You will be asked to disrobe (we will provide you with disposable underwear, if you wish). A series of pictures in three choreographed positions will then be captured in our completely private Melanoscan booth – the automated instructions will direct you through each simple step of the procedure. To facilitate the process we ask that ladies do not wear any makeup, any long hair is pulled up, and that watches and jewelry are removed.
After the images are captured, the dermatologist will examine you in the areas that are hard to image such as the oral cavity and the scalp. After the appointment, your dermatologist will review the images, and if anything is considered to need further attention you will be notified. Your dermatologist will recommend an appropriate time frame after which another series of images will be taken.
For more information on the revolutionary Melanoscan technology you may visit melanoscan.com
Dr. Rhett Drugge’s deep commitment to research and patient care with a special focus on physician to physician communications led to his founding of the Internet Dermatology Society. This society encourages members to share a data description language which facilitates access to dermatology information resources by common application programs and promotes uniform access to dermatology educational materials for Society members. It provides an Internetworked gateway for dermatology and the closely associated fields of, dermatologic surgery, dermatopathology and immunodermatology. The IDS assists dermatology societies and patient advocacy groups to use the Internet.
Through the Internet Dermatology Society an online “Electronic Textbook of Dermatology” is provided to its users. Dr. Drugge is the Founding Editor of this invaluable resource which has served millions of online users with information on topics in Dermatology since its inception in 1996.
The Internet Dermatology Society also has a feature called: Global Dermatology Grand Round. This is a tool for dermatologists and physicians to share their challenging cases with their peers.
Copyright ©2020 Sheard & Drugge, P.C.